Mamas Mamas m.mamas@keele.ac.uk
Do patients have a worse outcome with heart failure than cancer? A primary care based cohort study with 10-year follow-up in Scotland
Mamas
Authors
Abstract
Aims
This study was designed to evaluate whether survival rates in patients with heart failure (HF) are better than those in patients with diagnoses of the four most common cancers in men and women, respectively, in a contemporary primary care cohort in the community in Scotland.
Methods and results
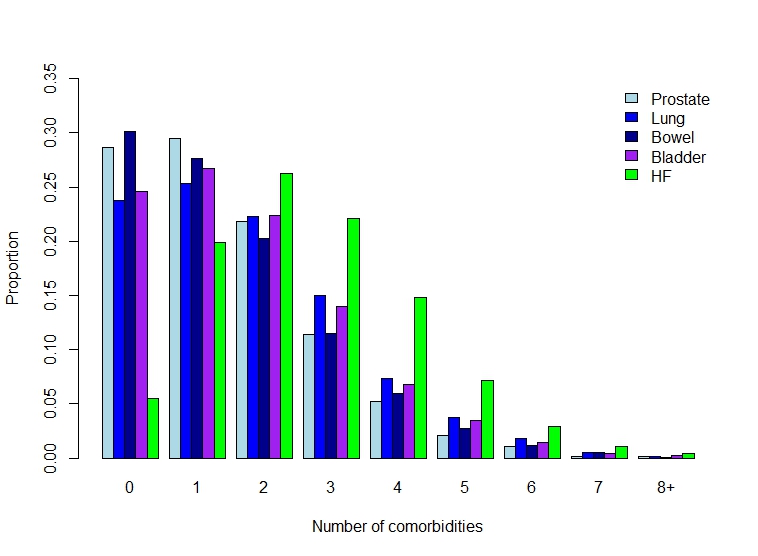
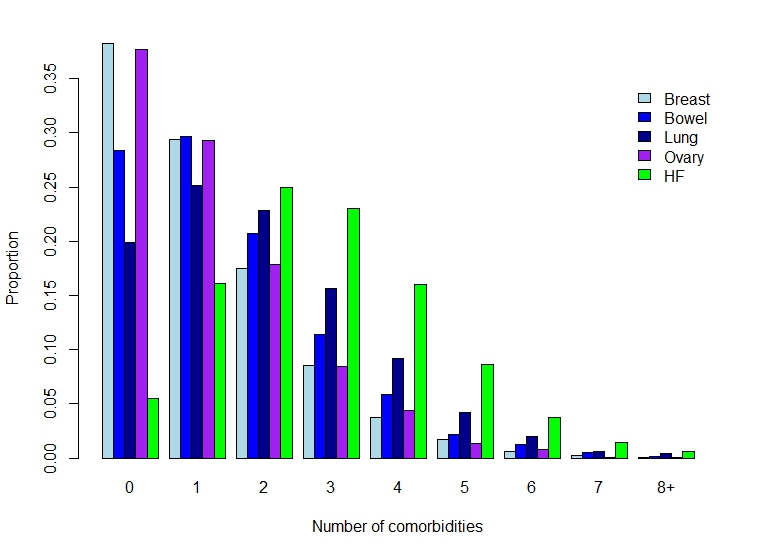
Data were obtained from the Primary Care Clinical Informatics Unit from a database of 1.75?million people registered with 393 general practices in Scotland. Sex-specific survival modelling was undertaken using Cox proportional hazards models, adjusted for potential confounders. A total of 56?658 subjects were eligible for inclusion in the study. These represented a total of 147?938 person-years of follow-up (median follow-up: 2.04?years). In men, HF (reference group; 5-year survival: 55.8%) had worse mortality outcomes than prostate cancer [hazard ratio (HR) 0.61, 95% confidence interval (CI) 0.57–0.65; 5-year survival: 68.3%], and bladder cancer (HR 0.88, 95% CI 0.81–0.96; 5-year survival: 57.3%), but better outcomes than lung cancer (HR 3.86, 95% CI 3.65–4.07; 5-year survival: 8.4%) and colorectal cancer (HR 1.23, 95% CI 1.16–1.31; 5-year survival: 48.9%). In women, HF (reference group; 5-year survival: 49.5%) had worse mortality outcomes than breast cancer (HR 0.55, 95% CI 0.51–0.59; 5-year survival 77.7%), but better outcomes than colorectal cancer (HR 1.21, 95% CI 1.13–1.29; 5-year survival 51.5%), lung cancer (HR 3.82, 95% CI 3.60–4.05; 5-year survival 10.4%), and ovarian cancer (HR 1.98, 95% CI 1.80–2.17; 5-year survival 38.2%).
Conclusions
Despite advances in management, HF remains as ‘malignant’ as some of the common cancers in both men and women.
| Acceptance Date | Feb 27, 2017 |
|---|---|
| Publication Date | May 3, 2017 |
| Journal | European Journal of Heart Failure |
| Print ISSN | 1388-9842 |
| Publisher | Wiley |
| Pages | 1095-1104 |
| DOI | https://doi.org/10.1002/ejhf.822 |
| Publisher URL | http://dx.doi.org/10.1002/ejhf.822 |
Files
Table 3 Final.doc
(42 Kb)
Document
Publisher Licence URL
https://creativecommons.org/licenses/by-nc/4.0/
Table 2 MS Final.doc
(100 Kb)
Document
Publisher Licence URL
https://creativecommons.org/licenses/by-nc/4.0/
Figure 1A.jpeg
(95 Kb)
Image
Publisher Licence URL
https://creativecommons.org/licenses/by-nc/4.0/
Figure 1B.jpeg
(97 Kb)
Image
Publisher Licence URL
https://creativecommons.org/licenses/by-nc/4.0/
mamas_heart_fail_feb_2017.pdf
(91 Kb)
PDF
Publisher Licence URL
https://creativecommons.org/licenses/by-nc/4.0/
Table 1 MS Final.doc
(100 Kb)
Document
Publisher Licence URL
https://creativecommons.org/licenses/by-nc/4.0/
Fig 2 HQ final.tif
(5.8 Mb)
Other
Publisher Licence URL
https://creativecommons.org/licenses/by-nc/4.0/
fig3HQ.tif
(5.8 Mb)
Other
Publisher Licence URL
https://creativecommons.org/licenses/by-nc/4.0/
You might also like
Downloadable Citations
About Keele Repository
Administrator e-mail: research.openaccess@keele.ac.uk
This application uses the following open-source libraries:
SheetJS Community Edition
Apache License Version 2.0 (http://www.apache.org/licenses/)
PDF.js
Apache License Version 2.0 (http://www.apache.org/licenses/)
Font Awesome
SIL OFL 1.1 (http://scripts.sil.org/OFL)
MIT License (http://opensource.org/licenses/mit-license.html)
CC BY 3.0 ( http://creativecommons.org/licenses/by/3.0/)
Powered by Worktribe © 2024
Advanced Search